2020B09 Discuss factors that influence the toxicity of local anaesthetics
when used for topical anaesthesia of skin and mucosa.
List:
· Means of toxicity
· Determinants of drug uptake
· Determinants of LAST susceptibility
Means of toxicity:
|
LAST |
· Systemic blockade of voltage-gated Na+ channels (∝ dose) · CNS effects: e.g. seizure, coma · CVS effects: e.g. arrhythmia, arrest |
|
Cocaine toxicity |
· Effects mostly ∝ dose · Effects ? additive ? synergistic with other local anesthetics (e.g. nasal surgery) · CVS: ↑↑noradrenaline -> ↑BP,
↑HR, coronary vasoconstriction, · CNS: ↑↑dopamine -> euphoria, risk-taking · Nasal: profound vasoconstriction -> ischaemic necrosis (∝ dose) |
|
Prilocaine toxicity |
· ↑Methaemoglobin -> Hb unable to bind O2 (∝ dose) · ↑↑Risk of reductase deficiency: neonate, congenital |
|
Hypersensitivity |
· i.e. allergy, anaphylaxis (dose-independent) · e.g. PABA metabolite of esters · e.g. sodium metabisulfite preservative with lignocaine |
Determinants of drug uptake:
|
Diffusion rate: |
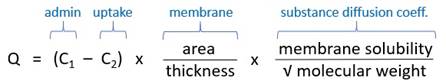
Fick’s law:
|
|
- ↑C1 |
· ↑Drug concentration (e.g. 10% lignocaine for airway topicalisation) · Eutectic mixture: optimal ratio -> ↓melting point -> liquid state -> ↑C1 (cf. solution) o EMLA: 2.5% lignocaine + 2.5% prilocaine, melting point 18°C |
|
- ↓C2 |
· ↑Tissue blood flow -> ↓C2 but also offset of local effect · Regional variation: e.g. lower flow to foot cf. scalp · Drug effect: e.g. prolonged EMLA application -> vasodilation · Drug additive: adrenaline -> ↓rate of absorption (e.g. nasal lignocaine) · Pathology: hypothermia, shock, heart failure |
|
- ↑Area |
· ↑Area of application ->
↑total absorption but ↔ absorption per unit area |
|
- ↓Thickness |
· Extensor thicker than flexor · Lower limb thicker than upper limb · Mucous membrane -> ↓↓thickness, ↑↑rate of blood flow o Contraindication for EMLA, topical amethocaine o Risk of inadvertent overdose during topicalisation for AFOI |
|
- ↑Diffusion coefficient |
· ↑Lipid solubility -(lignocaine 150x, prilocaine 50x procaine) · ↑% unionized o Drug: lignocaine 25%, prilocaine 33%, higher than most o Additive: NaOH in EMLA -> ↑pH · ↓Molecular weight (all LA drugs have similar MW 200-250g/mol) |
|
Diffusion time: |
· Uptake ∝ application time · EMLA 30 mins for PIVC, 120 mins for skin graft · 2% lignocaine viscous gargle < 1 minute for pharyngeal topicalisation |
Determinants of LAST susceptibility:
|
Drug |
Pharmacokinetics (PK): · Esters: rapid metabolism by BChE -> short t1/2β · Amides: slow metabolism by liver -> long t1/2β Pharmacodynamics (PD): · Toxicity threshold: bupiv 1.5mcg/mL, ropiv 4mcg/mL, lignocaine 5mcg/mL · CC:CNS ratio – bupivacaine 3:1, ropivacaine 5:1, lignocaine 7:1 |
|
Patient |
PK: · Absorption: see above · Distribution: Cachexia -> ↑plasma concentration -> ↑risk · Metabolism: liver disease -> ↓rate of amide removal -> ↑risk PD: · Class 1 antiarrhythmics -> ↑Na+ channel blockade -> ↑risk · CVS o ↑HR -> ↑channel cycling rate -> ↑risk o ↓PaO2, ↓pH, ↑K+ -> ↑risk o IHD, channelopathy -> ↑risk arrhythmias o AV conduction delay -> ↑risk high grade block from lignocaine · CNS o ↑PaCO2 (↑CBF), ↓PaO2, ↓pH -> ↑risk o Pregnancy -> ↑local anaesthetic sensitivity o Epilepsy, tramadol -> ↓seizure threshold |
Feedback welcome at ketaminenightmares@gmail.com