2021B06 Explain how local anaesthetics prevent the conduction of action potentials within a major peripheral nerve.
List:
· Nerve physiology
· Mechanism of action
· Differential effects
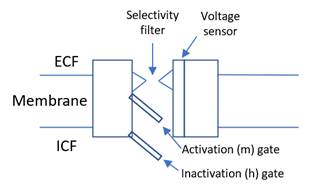
Nerve physiology:
|
Sodium channel |
|
||||||||||||
|
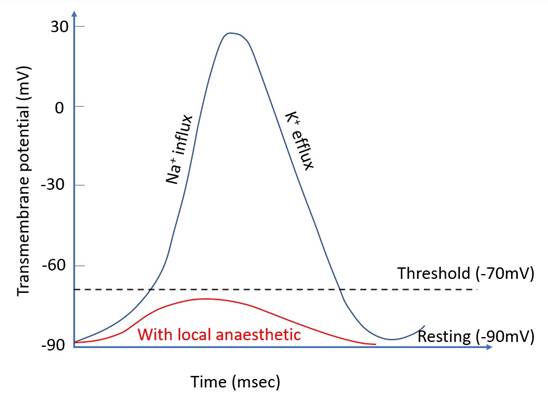
Action potential |
|
Mechanism of action:
|
· Voltage-dependent Na+ channel (VDNaC) · Less active at VDKC, VDCaC |
|
|
Entry |
· Spread across three consecutive nodes of Ranvier (if myelinated)
·
Diffusion across connective tissue and cell
membrane · Major: unionised form enters cell -> ionised form enters active receptor · Minor: ionised form enters active receptor from outside |
|
Binding |
· Rate of binding ∝ time in active state ∝ rate of cycling ∝ nerve activity · Affinity: inactive > resting > activated |
|
Effect |
· Reduced rate of cycling -> no action potential -> no signal propagation · No change to resting potential · Initial blockade: incomplete, tonic · Repeated blockade: complete, phasic |
|
Differential effect |
· ↑ Sensitivity if o Unmyelinated o Small o Active · Hence analgesia (C, Aδ) > sensory (Aβ) > motor (Aα) |
Feedback welcome at ketaminenightmares@gmail.com
Appendix: differential effects:
|
Type |
Function |
Size (μm) |
Conduction velocity (m/s) |
Myelination |
LA sensitivity |
|
Aα |
Motor Proprioception |
12-20 |
70-120 |
Heavy |
+ |
|
Aβ |
Light touch Vibration |
5-12 |
30-70 |
Heavy |
++ |
|
Aγ |
Tone Spindles |
3-6 |
15-30 |
Heavy |
+++ |
|
Aδ |
Sharp pain Cold temperature |
2-5 |
12-30 |
Heavy |
++++ |
|
B |
Pre-ganglionic: SNS and PSNS |
<3 |
3-15 |
Light |
++++++ |
|
C-polymodal |
Dull pain Warm temperature |
0.4-1.2 |
0.5-2.3 |
None |
+++++ |
|
C-SNS |
Post-ganglionic: SNS vasomotor |
0.3-1.3 |
0.7-2.3 |
None |
+++++ |