2016B06 Discuss the determinants and control of spinal cord perfusion.
List:
· Intro
· Flow dynamics
· Regular of vascular resistance
· Anatomical factors
Intro:
|
Physiology |
· Similar to brain tissue · Highly active: O2 consumption 3.3mL/min/100g · Highly perfused: 58mL/min/100g |
|
Pathology |
· Interruption -> ischaemia -> paralysis |
Flow dynamics:
|
Ohm’s law |
SBF = mAP – SCP or CVP / SVR · SBF: spinal blood flow · SCP: spinal cord pressure · SVR: spinal vascular resistance
Hence factors ↓CBF: · ↓ mAP · ↑ SCP / ↑ CVP (Starling resistor – whichever is higher) · ↑ SVR |
|
|
Poiseuille’s law |
Resistance = (8 x length x viscosity) / (π x radius4) – assuming laminar flow
Hence factors ↑resistance: · ↓Radius (note power of 4, most important) · ↑Length (not under control) · ↑Viscosity |
|
Regulation of vascular resistance:
|
Autoregulation |
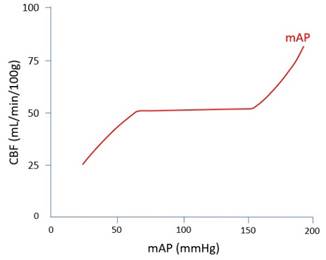
Myogenic: · Global blood flow constant 58mL/min/100g · ↑flow -> ↑stretch -> reflex contraction -> ↓radius -> ↓flow · Effective for perfusion pressure 50-150mmHg
Metabolic: · Regional blood flow ∝ metabolic rate (MR) · ↓MR -> ↓H+/K+/adenosine/lactate/pCO2 and ↑pO2 -> local vasoconstriction -> ↓radius -> ↓flow |
|
Physiological variables |
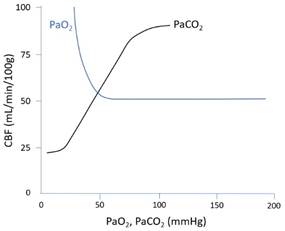
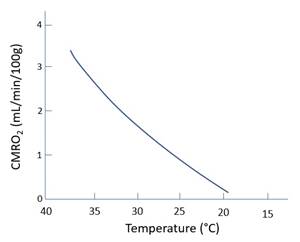
Oxygen: · ↓PaO2 <50mmHg -> vasodilate -> ↑radius -> ↑SBF · Non-linear response. Doubles at 30mmHg. Carbon dioxide: · ↑PaCO2 -> vasodilate · Linear response 20-80mmHg Temperature: · ↓Temp: ↓MR -> ↓SBF via metabolic autoregulation · Near linear response: ↓7% per 1°C
|
|
Other |
· Neural: noradrenaline at α1 -> vasoconstriction (minor) · Hormonal: adrenaline -> mixed effects at α1, β1 (minor) · Rheologic: ↑Hct -> ↑viscosity -> CVR |
Anatomical factors:
|
Arterial supply |
· Anterior spinal artery – anterior 2/3 (from vertebral arteries) · Posterior spinal artery x 2 – posterior 1/3 · Segmental reinforcement by thoracic and lumbar arteries ·
Major reinforcement by the artery of
Adamkiewicz (usually left T11) |
|
Venous drainage |
· Radicular veins · Anterior and posterior spinal veins · Internal vertebral venous plexus |
Feedback welcome at ketaminenightmares@gmail.com