2009A11 Outline the determinants and regulation of extracellular fluid volume.
List:
· Intro: body compartments and ECF volume determinants
· ECF volume sensors
· ECF volume controller
· ECF volume effectors
Intro:
|
Body fluid compartments |
· Body is 60% water (42L of 70kg) · 2/3 ICF (i.e. cytosol) 28L · 1/3 ECF (i.e. outside cells) 14L. ¼ plasma 3.5L, ¾ ISF 10.5L · (others: bone, dense CT, transcellular unimportant to fluid dynamics) · Note compartments are functional not anatomical |
|
Determinants of ECF volume |
1. Amount of Na+ in ECF (most important and controllable effective ECF osmole) a. Na+ alone: aldosterone b. Na+ and H2O: angiotensin 2, ANP 2. Tonicity of ECF a. Water intake: thirst b. Water output: ADH |
ECF volume sensors:
|
Via central blood volume |
· Low pressure baroreceptors in walls of atria and great veins · Stretch-activated mechanoreceptors · Activation of receptor results in inhibitory signal via CNX afferents |
|
Via systemic arterial pressure |
· Carotid and aortic sinus baroreceptors · ↓mAP -> ↓stretch -> ↓inhibition of output to hypothalamus via CNIX (carotid) and CNX (aortic) |
|
Via renal afferent arteriolar pressure |
· Renal baroreceptors · ↓mAP -> ↓stretch -> ↓inhibition of granular cell -> ↑renin release |
ECF volume controller:
|
Brain |
· Hypothalamus controls ECF sodium content and tonicity |
|
Kidney |
· Juxtaglomerular apparatus controls ECF sodium content |
ECF volume effectors:
|
RAAS |
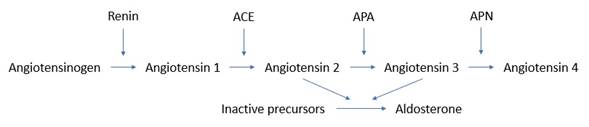
· Stimuli for renin release: o ↑SNS activation of granular cells (β1) o ↓stretch of afferent arteriolar baroreceptors o ↓NaCl delivery to macula densa · Stimuli for aldosterone release: o ACTH o Angiotensin 2 o ↑K+ · Actions of angiotensin 2: o Renal: § ↑Activity proximal tubule Na+/H+ exchanger § ↑Na+/H2O/HCO3- reabsorption § ↑ECF volume and pH o Vascular § Peripheral vasoconstriction -> ↑SVR, mAP § Constriction of efferent > afferent -> ↑GFR § Constriction of peritubular capillaries -> ↑reabsorption o Hypothalamic § Thirst § ADH release · Actions of aldosterone (most important factor): o Na+ reabsorption from connecting tubule and collecting ducts (MR) o Na+ reabsorption from colon, sweat glands (MR) o ↑ECF tonicity directly o ↑ECF volume indirectly (↑osmolarity -> ↑ADH release) · Negative feedback: o Direct: AT2 binds AGTR1 on granular cell -> ↑Ca2+ -> ↓renin release o Physiological: effects of AT2 and aldosterone -> ↓renin release |
|
ANP |
· Stimulus: o Distension of right atrium (i.e. ↑central blood volume) · Effects: o Dilatation of afferent arteriole, constriction of efferent arteriole -> ↑GFR o Inhibit NCC in distal tubule, ENaC in connecting tubule and collecting duct -> ↓Na+/H2O reabsorption o i.e. natriuresis o ↓ECF volume |
|
ADH |
· Production: hypothalamus (supra-optic and paraventricular nuclei) · Release: posterior pituitary · Stimuli: o ↑osmolality (sensitive to ∆2%) o ↓BV (sensitive to ∆10% i.e. ↓BV 0.5L, ↓ECF 1.4L, ↓TBW 4L; overrides osmolarity) o ↓mAP o Angiotensin 2 o Stress (e.g. surgery) o Drugs (e.g. SSRI) · Effects: o Insertion of aquaporins into collecting duct apical membranes (↑free H2O reabsorption) o Insertion of ureaporins into medullary collecting duct apical membranes (↑medullary interstitial osmolarity) o (Other: generalized vasoconstriction, ↑ACTH release) o ↑ECF volume and ICF volume |
|
Thirst |
· Stimuli: as for ADH (except for stress response and drugs) o ↑Osmolality o ↓Blood volume o ↓mAP o Angiotensin 2 at SFO and OVLT · Effect: o ↑free water intake o ↑ECF volume and ICF volume |